Downloaded from www.mymenopausecentre.com
Direct URL: https://www.mymenopausecentre.com/symptoms/sleep-issues/
Menopause and sleep issues
Sleep issues are common and are often a result of ageing. Poor sleep may be linked to hormone changes, but physical symptoms, like hot flushes, mood changes, and stress can contribute too.
Explore
Book an appointment
The highly experienced doctors and nurses in our menopause clinic are here to help you. Appointments from £190.
Book An AppointmentIf you would like to learn more about the impact of your symptom(s) complete our free online menopause questionnaire here.
What are menopause-related sleep issues?
Women often talk to us about how difficult they’re finding it to get a decent night’s sleep. The effects of sleep issues can be debilitating and can take their toll on your daily life, affecting your mood, behaviour and even your long-term health.
Studies have also shown that lack of sleep can affect mood, making your brain focus on negative thinking, and also leading to a tendency for your brain to remember unhappy events rather than happy ones[1].
Your judgement and concentration can be impaired, which doesn’t help the experience of menopausal brain fog. Inadequate sleep can also affect your behaviour, so that you may take more risks. Reaction time decreases, and you can become more accident-prone and clumsy.
If you’re struggling with sleep, we hope this information will encourage you to ask for help if you need it.
What causes sleep issues?
There are many reasons why sleep can be affected by the menopause. To understand why and how let’s first look at the whole process of sleep.
Understanding sleep
When you’re asleep, your brain cycles through two different types of sleep – REM (rapid eye movement) and non-REM sleep.
Non-REM sleep comes in four stages:
- Stage 1: the first is between asleep and awake
- Stage 2: the second is light sleep when your heart rate and breathing regulates, and body temperature drops
- Stage 3 and 4: the third and fourth stages are deep sleep, when your body restores itself and the brain drops its activity
Non-REM sleep is essential for learning and memory and is more restful and restorative.
Here’s how a typical sleep pattern looks:
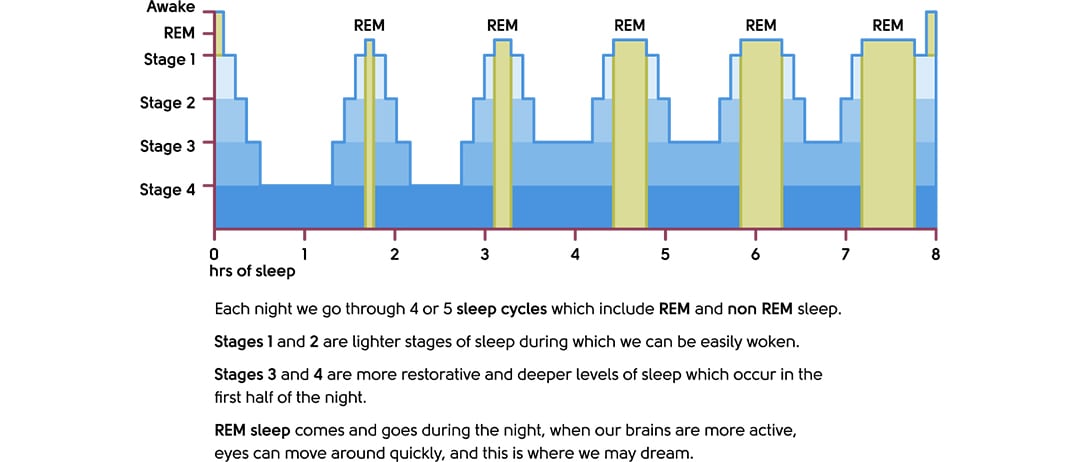
Illustration to show the sleep cycle and different stages of sleep
You’re more likely to wake with hot or cold sweats during REM sleep because it’s the lightest. Stage 3 and 4 non-REM sleep is the deepest sleep and is the most restorative.
Sleep and the menopause
There are many reasons that the menopause affects your sleep. Broken sleep can be directly connected to some of the physical symptoms of the menopause – for example, being woken up in the night by hot flushes and night sweats, or joint pains.
You may also need to get up in the night to go to the loo to pass urine – something you didn’t do before the menopause transition.
Psychological symptoms, such as anxiety and increased stress, can leave you tossing and turning. We know that sleep is affected by low mood and depression too.
Sleep apnoea is when your breathing stops and starts while you sleep, causing snoring and snorting due to the partial obstruction of the upper airways. It’s typically found in women who are overweight – but not always. It can increase after the menopause because of a direct effect of changing hormones, and is not just a factor of weight.
Sleep apnoea can cause headaches, anxiety, low mood, and tiredness. If you think you may have sleep apnoea, you should speak to your GP who can refer you to a specialist.
Many women ask us about melatonin and sleep. Melatonin is a hormone that’s important for our sleep/wake cycle. Melatonin levels decrease in both men and women as we get older. It could be a factor affecting your sleep during the perimenopause and menopause. Melatonin seems to be important in sleep timing (reminding your body that it’s time to sleep) and promoting sleep – but it’s not a sedative.
Although the changes in hormones are thought to play an important part in causing sleep problems, it’s probably not the complete picture, as sleep quality declines with age in men and women.
Other factors that are important in affecting sleep:
- Alcohol can get you off to sleep, but the resulting quality of sleep can be poor. You experience a lighter sleep and don’t feel rested when you wake
- Caffeine in tea and coffee is a stimulant – drinking caffeine before bed, or having too much during the day may keep you awake at night
- Conditions such as chronic pain and some medication can affect sleep
- Obesity can also cause sleep issues, including sleep apnoea (see above – some women find that sleep apnoea increases after the menopause)
- Smoking can cause difficulty with sleeping as nicotine is a stimulant
How many women typically experience sleep issues?
In research conducted by the British Menopause Society, up to 60% of the women interviewed mentioned sleep problems [2].
Are sleep issues linked to any particular stage of the menopause?
Sleep issues can occur during any stage of the menopause transition. Ageing can also be a factor, so sleep may continue to be a challenge in postmenopausal life.
How can sleep issues be treated?
There are many things that can help with sleep issues, and here are a few tips. Always seek help from your doctor or a healthcare professional if sleep issues are really affecting your life.
Managing stress and worry
Stress and worry about sleep can be a problem for some. Tackling these negative thoughts can help.
Knowing that you’ve had the most restorative sleep (during the first part of the night) can help some people. If you wake in the middle of the night, knowing that your body has had a chance to repair may take away some of the worries about not sleeping, and you may even go back to sleep again. It’s normal to wake several times a night and most people do not need eight hours of sleep.
Avoid limiting your daytime activities because of poor sleep. Instead, pace yourself and try to carry on as normal so that your life doesn’t shrink because of lack of sleep. You may be surprised at how much you can do in manageable chunks – and this means that you are more likely to go to bed tired at the end of the day, as well as being able to live your life.
Managing your sleep environment
Making sure your sleep environment is geared up for a good night’s sleep is important:
- First of all, make sure your bedroom is cool and dark, as it can make all the difference. Cooling cotton sheets and a good choice of nightwear can also help
- Get into a bedtime routine that involves time away from screens. Try to keep your bedroom for sleep (and not working, scrolling on your phone or watching TV)
- If you’re tossing and turning in the night, get up for a while – you’re trying to train your brain to associate your bedroom with sleep
- Try to avoid going to bed too early, which often means that you’ll lie awake for long periods in bed. If you do wake in the night, consider going to another room and doing something gentle and soothing. Then try going back to bed when you feel tired
Lifestyle factors
- Avoid large meals that are rich in heavy or spicy foods before you go to bed
- Try to avoid caffeine for at least four hours before bed, or from the early afternoon, as this is a stimulant
- Try to limit how much alcohol you drink in the day. Alcohol is also a stimulant and decreases sleep quality, so avoiding this may help
- Try to stop smoking as it’s also a stimulant (and not good for your health)
Hormone Replacement Therapy (HRT)
You might think HRT is best placed to tackle the physical menopause symptoms (like hot flushes) that can cause sleep issues. It’s true, HRT can help with physical symptoms, but it can also have a direct effect on your overall quality of life, energy levels, and sleep[3].
You may feel anxious about taking HRT because of the well-publicised small risks, particularly of breast cancer. In reality, these risks are tiny for most. Lifestyle factors, like how much you weigh and how much alcohol you drink, can have a greater impact on your risk of breast cancer than HRT.
You can find out more about HRT here.
Cognitive behavioural therapy (CBT)
Cognitive behavioural therapy (CBT) can help some women. The process works by challenging the negative thought processes surrounding lack of sleep and teaches strategies for turning around your negative thinking. You can find out more about our CBT partners Sue Makin and Claire Lloyd.
Sleep tips from Dr Clare Spencer
What next?
If you’re troubled by sleep issues, talk to your GP, or book an appointment with our menopause clinic, to talk about your symptoms in the context of the menopause.
If you think you may be experiencing symptoms of the menopause transition, you can learn more with our symptom checker or by taking our Menopause Questionnaire.
You can also find more information about the menopause transition at the British Menopause Society and the National Institute for Health and Care Excellence.
Authored by:
Dr Clare Spencer
Registered menopause specialist, GP and co-founder.
Last updated:
18/01/2024
Book an appointment
The highly experienced doctors and nurses in our menopause clinic are here to help you. Appointments from £190.
Book An AppointmentLearn more
Join the pause. community
We’ve created pause. as a space for women to come together and share stories about their menopause experience, ask questions, and to find support and inspiration. We'll also share the latest news and updates on the menopause from our experts.
Want to be the first to hear our latest news? Join our pause. community today.
Share your email to receive the latest news, updates and information on new products and treatments from My Menopause Centre and our pause. community. You can unsubscribe at any time.
We're committed to protecting and respecting your privacy - see our Privacy Policy and Terms and Conditions

Book a consultation
Whether you want to discuss your symptoms, create a treatment plan that's right for you, understand some test results or have a check-up, the highly experienced doctors and nurses in our menopause clinic are here to help you.
Book nowReferences
-
Source: Krause AJ, Simon EB, Mander BA, Greer SM, Saletin JM, Goldstein-Piekarski AN, Walker MP. The sleep-deprived human brain. Nat Rev Neurosci. 2017 Jul;18(7):404-418.
-
Source: Currie H, Moger SJ. Menopause – Understanding the impact on women and their partners. Post Reproductive Health. 2019;25(4):183-190.
-
Source: Newson, LR. Best practice for HRT: unpicking the evidence.Br J Gen Pract 2016; 66: 597–598.
Contact My Menopause Centre
- General enquiries: hello@mymenopausecentre.com
- Book appointments online: Log into your account and go to 'My appointments'
- Book appointments by phone: 0333 444 1067
- Website: https://www.mymenopausecentre.com