If you would like to learn more about the impact of your symptom(s) complete our free online menopause questionnaire here.
What is menopause-related vaginal dryness, itching and irritation?
Vaginal dryness is a very common symptom of the menopause. Many women find that they only feel dry during sex, while others experience it daily. Dryness comes with other sensations, such as ‘prickliness,’ itching, irritation, and even pain in the vagina.
Vaginal dryness can make you more prone to yeast infections (thrush), as the tissue is delicate and loses its natural defences. Discharge can decrease or increase as the balance of bacteria that are naturally found in the vagina changes.
You may also be more prone to bacterial vaginosis, where there is an imbalance of the normal bacteria that usually live happily in the vagina. If you have excessive vaginal discharge, this can sometimes cause further irritation.
What causes vaginal dryness, vaginal itching and irritation?
Oestrogen is needed to keep tissues well lubricated, healthy, and stretchy. Loss of oestrogen in the perimenopause and menopause results in the tissues becoming delicate and dry.
In addition, the usual elasticity of the vagina and vulva can be lost, which can lead to painful sex. The vagina can become shorter and lose its usual folds. These changes are called urogenital atrophy.
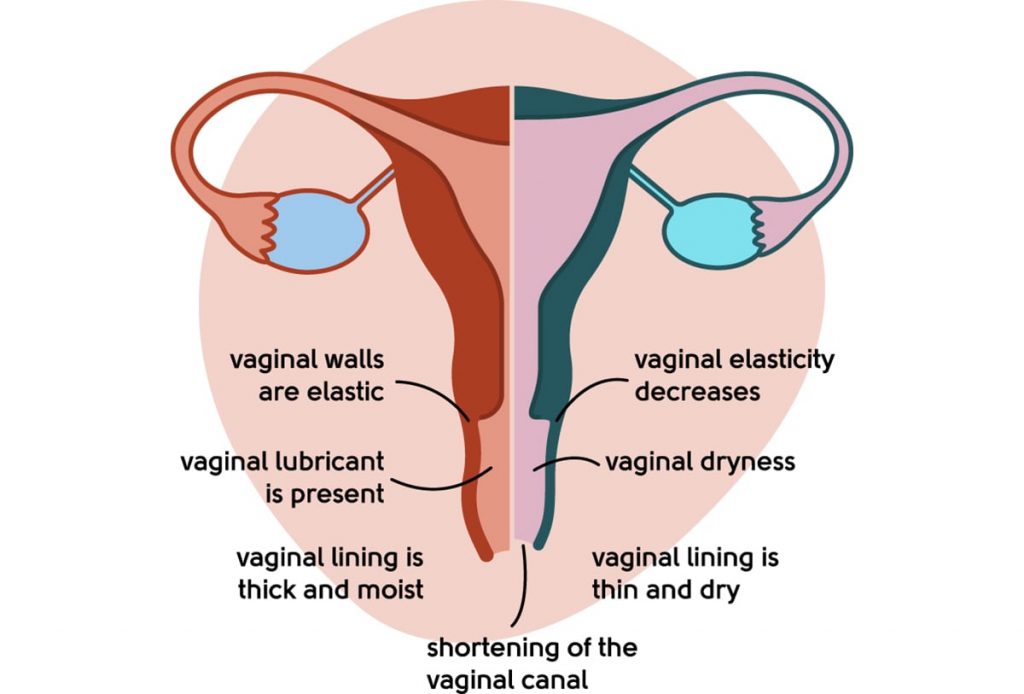
Illustration to show a healthy vagina vs urogenital atrophy
How many women typically experience vaginal symptoms?
In research conducted by the British Menopause Society, over one-third of the women interviewed experienced vaginal dryness, and over one in ten experienced pain during sex [1].
Vaginal symptoms become increasingly common as you age. Approximately two-thirds of postmenopausal women who haven’t taken HRT suffer from changes in the vagina and bladder linked to low oestrogen[2].
Studies also show that up to one-quarter of women using systemic HRT will still experience symptoms of urogenital atrophy[3].

Is vaginal dryness, vaginal itching, and irritation linked to any particular stage of menopause?
While vaginal symptoms of urogenital atrophy become more common with age, they can occur at any stage of perimenopause and menopause.
How can vaginal dryness and vaginal itching and irritation be treated?
Even though vaginal changes are common throughout the menopause transition and are a natural part of the ageing process, there are things that you can do to help with dryness, itching and irritation.
Lubricants
You’ll probably find it a good idea to start using lubrication during sex. Oil-based ones can be more effective – though they can make condoms less effective. You can also buy water-based and silicone-based lubricants. The key thing is finding one you like.
You should avoid the lubricants with added extras (like a tingle, or heat) as they can cause more irritation.
Moisturisers and washing
You can buy vaginal moisturisers over the counter and they can help with day-to-day symptoms. We recommend that you avoid anything perfumed, because, again, they can cause further vaginal irritation.
You’ll most likely find it best to avoid all soap when it comes to washing, as it often dries out already delicate and sensitive skin. Instead, try using a soap-free wash, or even over-the-counter emollient creams and ointments. If you ask the pharmacist, they will be able to point you in the right direction.
Hormone Replacement Therapy (HRT)
Systemic HRT (patches, tablets, gels and sprays) helps some women, but not everyone and up to one-quarter of women using HRT will also need a vaginal oestrogen[4]. More on that below. You can find more detailed information about the benefits and risks of HRT here.
Vaginal oestrogens
Vaginal oestrogens (topical oestrogens) can benefit you and are prescribed by your doctor. These are oestrogen pessaries, creams and gels that are inserted directly into the vagina.
Women often ask about the safety of using oestrogen. It’s reassuring to know that when you put oestrogen directly into your vagina, your body only absorbs a tiny amount. So you can use it without risk of breast cancer, blood clots, stroke or heart disease[5].
There are different options available for vaginal oestrogens, shown in the table below. The dosing varies for all of them and will be confirmed on your prescription. They may take at least three months to work. If you feel they aren’t working, always speak to a doctor who can then look for other causes of your symptoms.
| Vagifem TM |
Tiny pessary of 10mcg oestradiol with single use applicator for each pessary. |
| Vagirux TM |
Tiny pessary of 10mcg oestradiol with 1 applicator for re-use. |
| Gina TM |
Tiny pessary of 10mcg oestradiol with single use applicator for each pessary – available to buy over the counter for women who meet set criteria. |
| Imvaggis TM |
Small pessary of 0.03mg oestriol. No applicator – you insert it yourself into the vagina. Melts, which some women find moisturising. |
| Ovestin cream (Estriol 0.1%) TM |
Cream containing oestriol 1mg/g. Comes with a washable applicator, but you could measure out the applicator dose and use your finger instead. |
| Estriol 0.01% cream |
Cream containing 0.01% oestriol. Comes with a washable applicator, but you could measure out the applicator dose and use your finger instead. |
| Blissel TM |
Gel containing 50mcg/g oestriol. The lowest dose of vaginal oestrogen. This comes with an applicator. |
| Estring TM |
A flexible ring that delivers 7.5mcg oestradiol per 24 hours, that is fitted into the vagina, releasing oestrogen for three months. You can still continue to have sex with this fitted. |
Gina
Gina is essentially the same as Vagifem and Vagirux – 10mcg oestradiol pessaries with an applicator to help insert them. There are more restrictions in place to buying Gina over the counter than there are to getting the same medication on prescription from your doctor. Gina is available to buy to help manage vaginal symptoms of dryness, soreness, itching, burning and painful intercourse if:
- you are 50 years or older
- your period stopped more than 1 year ago
If you are already taking systemic HRT (for example HRT in patches, gel, spray or tablet form), the pharmacy can only sell you Gina if you have already been prescribed it by your doctor or if your doctor has confirmed that you are suitable to use an additional vaginal oestrogen.
If you are under 50, still having periods or it is less than a year since your last period, or if you are taking HRT, it is likely that you will still be able to use a vaginal oestrogen, but you would need to talk to your GP about your symptoms to obtain this on prescription.
You can find more information on Gina here.
Other medications
There are two other medications used to treat vaginal symptoms related to urogenital atrophy of menopause. They are usually prescribed by specialists.
- Prasterone (Intrarosa TM) is a pessary. It’s identical to a hormone called dehydroepiandrosterone (DHEA) in the adrenal gland. DHEA helps produce other hormones, including testosterone and oestrogen. This has been shown to be effective in treating menopausal vaginal and vulval atrophy (thinning) that is ‘moderate to severe’[6].
- Ospemifene (Senshio TM) is a tablet that is swallowed. It’s not an oestrogen, but has an oestrogen-like effect on the vagina, helping treat menopausal atrophy.
If you are worried that you have thrush or bacterial vaginosis
It’s always a good idea to speak to a doctor about your symptoms. A yeast infection (or thrush) can cause itching or itchy thick, white discharge, or no symptoms at all. You may think that you have thrush but the symptoms may be due to lack of oestrogen. If your symptoms are persistent a doctor may take a swab of the vaginal discharge. You can buy an over-the-counter thrush treatment in the form of pessaries (which are inserted into the vagina), cream or oral capsules. Speak to the pharmacist to ensure the medicine is safe for you. Always see a doctor if the over-the-counter treatment has not worked.
Bacterial vaginosis (BV) causes a fishy-smelling discharge, particularly after sex. It does not usually cause itching, but your vaginal discharge may be greyish white, thin and watery. Like thrush, you may not have symptoms. Bacterial vaginosis can be diagnosed by your GP or sexual health clinic. It is usually treated with antibiotic cream or tablets.
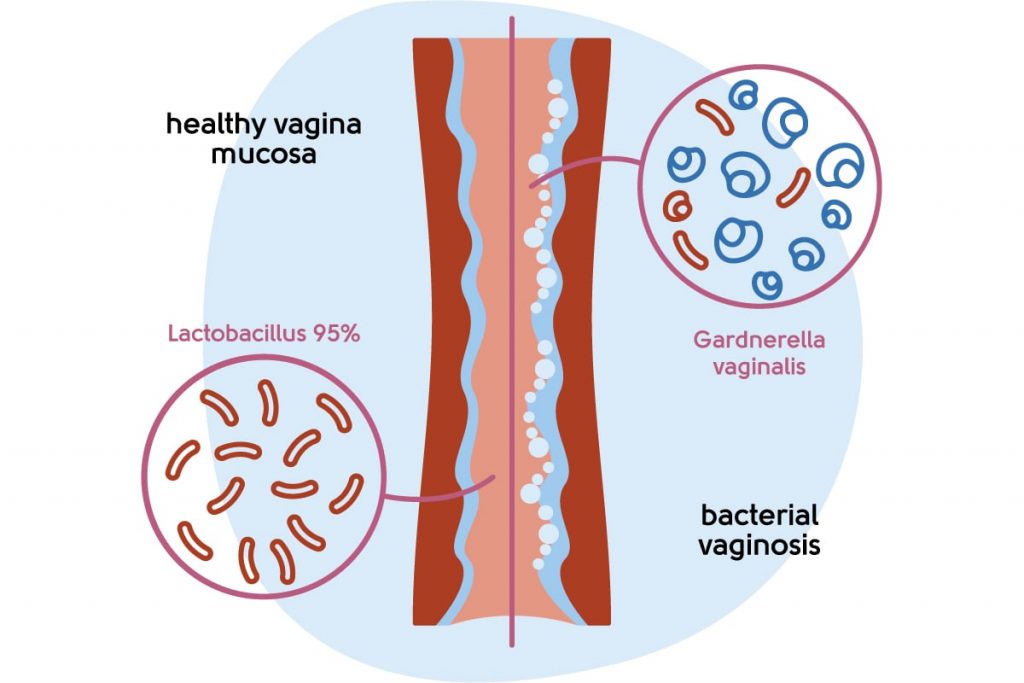
Illustration to show the bacterial imbalance in bacterial vaginosis
Vaginal laser treatment
Vaginal laser therapy is a technique that may help the symptoms of vaginal atrophy. Laser energy is used to treat the vaginal tissue and increase collagen production. Results from small studies have shown that this treatment can be effective but it is not yet widely available.
What next?
If you’re concerned about vaginal dryness, itching or irritation, see your GP, gynaecologist, or book an appointment with our menopause clinic.
If you think you may be experiencing symptoms of the menopause transition, you can learn more with our symptom checker or by taking our Menopause Questionnaire.
You can also find more information about the menopause transition at the British Menopause Society and the National Institute for Health and Care Excellence.